What Are the Signs Your Wisdom Teeth Need to Come Out?
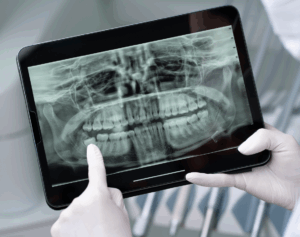
What are Wisdom Teeth and do you need them removed?
If you experience gaps closing between your teeth, pain, swelling or pressure in your jaw, pressure between or around your back teeth, looseness in your teeth, pain in your sinus cavity, and even radiating into your ear, it may be time to visit a dentist. The third set of molars, known as wisdom teeth, emerges during late teenage years and early twenties. Their novel name is deceiving though as they tend to create more problems than benefits for numerous people. When your wisdom teeth come in, they often begin to press on your surrounding teeth, pushing them closer together and causing those unpleasant symptoms above. According to the ADA, 60% of wisdom teeth will need to be extracted to prevent symptoms and damage to the surrounding teeth and gums.
Common Signs You May Need Wisdom Teeth Removal
- Persistent pain or pressure the back of your mouth or jaw
- Swollen, red, or bleeding gums around the molars
- Headaches, jaw stiffness, or discomfort when chewing
- Crowding or shifting teeth, especially if you’ve had braces
- Recurring infections or difficulty opening your mouth fully
The presence of impacted wisdom teeth becomes evident through these symptoms because they grow at unusual angles or stay hidden under gum tissue.
The Process
When you are searching for a dentist, it is wise to ensure that the practice you choose:
- Offers the services that you think you need (like wisdom tooth extraction)
- Is in network with your dental insurance (or will submit dental claims on your behalf)
- Offers sedation options
- Doesn’t have a long waitlist for the procedure you think you need (Many dental offices are booked out months in advance for procedures like wisdom tooth extractions)
Once you determine these things, the Dental Practice will schedule an appointment for you, typically an Emergency Exam. This exam ranges in price so be sure to ask about that when you call. The Emergency Exam involves an exam and a series of X-Ray’s, specifically looking at the area you are concerned with. From these images, they will be able to determine if your wisdom teeth need to be extracted, how soon, and what kind of extraction process you will need. If the wisdom teeth are impacted or a more advanced type of extraction is needed, the office may refer you to an Oral Surgeon.
Sedation Options
The dentist and their team will also go over your different sedation options, which can vary. Many dental practices offer inhaled Nitrous Gas as a sedation option, but some specialty offices will offer oral sedation, or IV sedation as well. Ask questions and consider the level of comfort you wish to have, what options are covered by your insurance, and what the associated costs are. It’s important to ask these questions if you want a sedation option during the surgical procedure.
How many need removed?
Another thing to consider, is how many wisdom teeth you plan to have extracted. Typically they don’t all begin to hurt at the same time. They can come in individually, or all together. It is recommended to remove both upper, both lower, or all 4 at the same time typically, to prevent further pain and damage to the surrounding teeth. Keep in mind, the process of preventive removal produces better results than waiting for more complications to develop.
What Happens If You Don’t Remove Them?
The failure to remove problematic wisdom teeth results in multiple dental and health complications which include
- Damage to nearby teeth or roots
- Cyst formation around impacted teeth
- Infections that spread to other areas of the mouth or jaw
- Increased risk of tooth decay and gum disease
How Long Does Wisdom Teeth Surgery Take?
Typically, wisdom teeth removal takes between 30 minutes and 1 hour per tooth. In some cases, it may take longer if the teeth are impacted or difficult to access. The recovery period for most patients lasts between 3 to 7 days before they can resume their normal activities.
What to Eat After Wisdom Teeth Removal
Your healing gums need soft foods which avoid causing any discomfort. The following list includes safe and satisfying food options for your recovery:
- Mashed potatoes, scrambled eggs, mac and cheese
- Applesauce, yogurt, pudding, and Jell-O
- Smoothies with no seeds! Milkshakes and protein drinks
- Oatmeal, cream of wheat, or soft rice
- Broths, pureed soups, soft tofu, and cottage cheese
- Avocado, ripe bananas, and well-cooked pasta

What Is Dry Socket and How to Prevent It?
The extraction site develops dry socket when the blood clot dislodges from its position. The condition leads to painful symptoms, infection, vomiting, and bleeding which can be avoided through proper care. It is imperative that you avoid smoking, drinking through a straw, and all foods that are hard to chew, crunchy, or spicy for at least seven days so that you do not get dry sockets.
- Do not smoker
- Do not use straws
- Do not spit forcefully
- Stick to your post-op instructions carefully
- Rinse gently with salt water starting 24 hours after surgery
You should contact your dentist immediately when you experience any unusually symptoms, including severe pain, bleeding, fever, nausea, vomiting, or unusual and unpleasant mouth odors as these could be symptoms of infection or dry sockets.
FAQ
How can I stop wisdom tooth pain at home?
Try rinsing with salt water, applying a cold compress, or taking OTC pain relievers like ibuprofen. If pain persists, you’ll need a dental exam.
Which symptoms indicate that a wisdom tooth has become infected?
The following symptoms indicate an infected wisdom tooth: Swelling, pain, bad taste, pus, fever and limited mouth opening. You should visit a dentist immediately when you notice these symptoms.
Can wisdom teeth cause jaw stiffness or soreness?
Yes! impacted teeth often cause tightness or aches in the jaw, especially when chewing or waking up.
What are the risks of not removing impacted wisdom teeth?
Delaying removal can lead to infections, damage to nearby teeth, cysts, and long-term jaw issues which aren’t fun.


 Review Us
Review Us  Review Us
Review Us  About Insurance
About Insurance 